- Fact Checked
- February 04, 2026
- 16 min read
Can IUDs Cause Yeast Infections?
Table of Contents
Table of Contents
If you have a vagina and are of reproductive age, you’re likely quite familiar with vaginal yeast infections. Yeast infections, also known as vaginal candidiasis or candida, are the second most common vaginal infection, infecting 75% of women at least once in their lifetime.
But for 45% of these women, these infections are not a one-off occurrence. For this 45%, vaginal yeast infections are recurrent, meaning they continue to happen over and over despite treatment.
If you are part of this 45%, you are probably feeling frustrated, to say the least, and trying to pinpoint the cause of your infections so you can finally put a stop to them. You may have also heard that using an IUD or intrauterine device for birth control can increase your risk of developing vaginal candidiasis. But is this actually true?
Long story short, it is. A study published in 2022 compared the use of hormonal and non-hormonal IUDs and the risk of developing yeast infections1. They took swab samples from 160 women 3 months after they received an IUD insertion and found that about 30% of women using copper IUDs had vaginal candidiasis, as did almost 23% of women using hormonal IUDs.
But does that mean IUDs should be avoided? No. The story is a little more complicated with that2. IUDs are still an excellent birth control option for many women. All contraceptive methods have pros and cons, and understanding what these are when it comes to IUDs will help you make more informed choices.
This post is for informational purposes only and does not constitute medical advice. See full disclaimer below.
What Is an IUD?
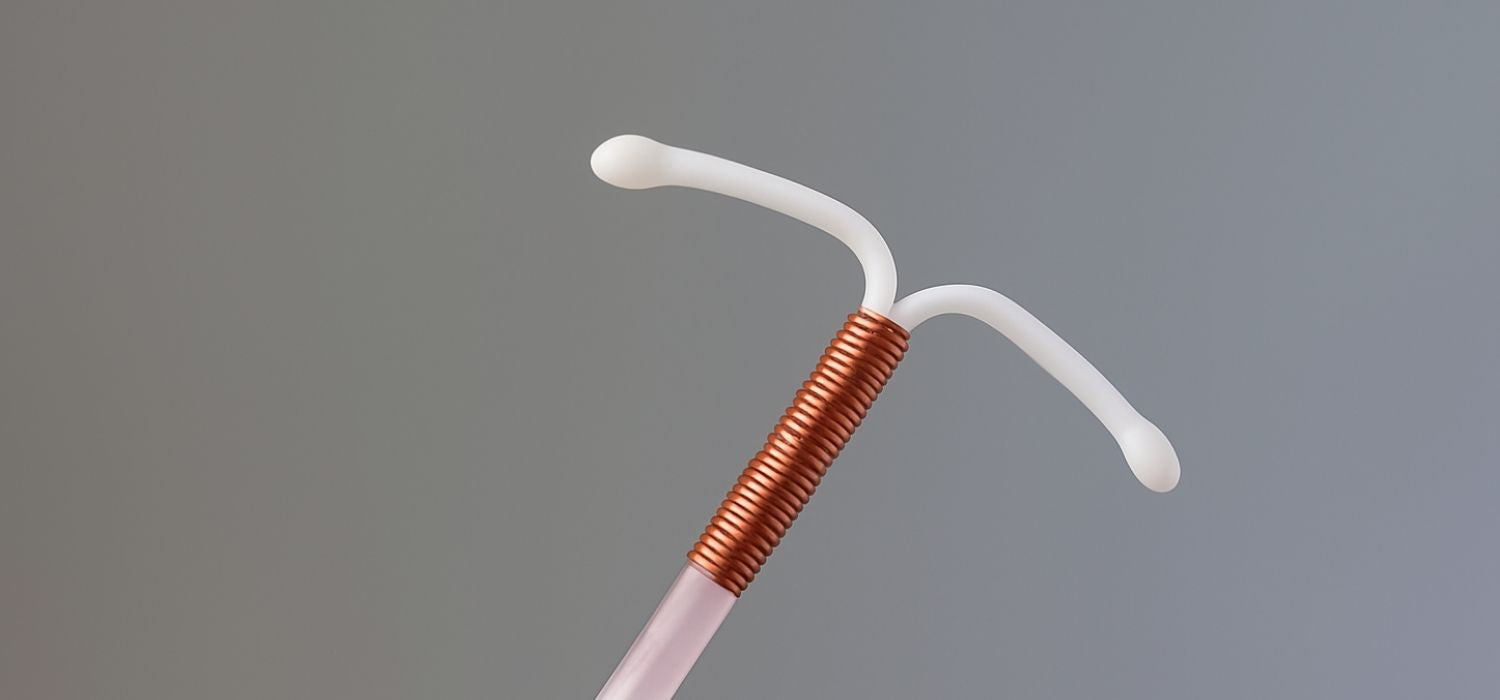
An IUD, or intrauterine device, is a small T-shaped contraceptive device that your OB/GYN or healthcare professional inserts into your uterus to prevent pregnancy3. They're made of either plastic or copper and come in two main varieties: hormonal and non-hormonal.
Both types are incredibly effective as methods of contraception. According to U.S. Selected Practice Recommendations for Contraceptive Use, hormonal IUDs have a failure rate of less than 0.02%, while copper IUDs clock in at less than 0.08%4. Compare that to birth control pills, which have a typical-use failure rate of about 7%, and you can see why IUDs have become such a popular birth control method.
Like all contraceptive devices, IUDs do come with potential side effects5. But for many women, these side effects are worth it for the peace of mind and convenience.
Non-Hormonal (Copper) IUDs
Copper IUDs don't contain any hormones. Instead, the copper itself prevents pregnancy by creating an inflammatory response in the uterus that's toxic to sperm and eggs6.
Copper IUDs start working immediately after insertion and can remain effective for up to 10 years. This makes them popular among women who've already had children or are done growing their families7. But they're also used by women of all reproductive stages and can even work as emergency contraception if inserted within 5 days of unprotected sex.
However, copper IUDs do have a higher association with yeast infections compared to hormonal options8. The copper ions released by the device trigger inflammatory responses that can disrupt your vaginal microbiome, particularly in the first year after insertion.
Common side effects include heavier menstrual bleeding (especially in the first few months after insertion), more intense cramps, and higher rates of bacterial vaginosis and candida or yeast infections9.
Hormonal IUDs
Hormonal IUDs release a synthetic hormone called progestin (levonorgestrel), which mimics your body's natural progesterone10. This hormone prevents pregnancy in two ways:
- It thickens cervix mucus to block sperm from reaching and fertilizing eggs
- It thins the uterine lining, making it harder for fertilized eggs to implant
While research suggests hormonal IUDs like Mirena may carry slightly less risk than copper options, studies show that candida prevalence in vaginal samples can actually increase during years 4 to 7 of use compared to the first year after insertion, hinting that over time, this hormonal birth control can impact the vaginal microbiome away from more protective bacteria.
Common side effects of hormonal IUDs include:
- Irregular bleeding or spotting (which can raise vaginal pH and create an environment where yeast thrives)
- Missed periods
- Higher risk of ectopic pregnancy (if pregnancy does occur)
- Increased risk of pelvic inflammatory disease (PID)
- Potential uterine perforation
- Increased prevalence of vaginal candidiasis and bacterial vaginosis
Keep in mind that while hormonal IUDs protect against pregnancy, they don't protect you from STIs or STDs—and neither do copper IUDs! Always use condoms with new or multiple partners to protect yourself from chlamydia, gonorrhea, and other infections.
What Are Yeast Infections?
Let’s cover another important basic before we move on: vaginal yeast infections (also called vaginal candidiasis, vulvovaginal candidiasis, or vaginal thrush) are the second most common vaginal infection. The CDC estimates they account for 1.4 million healthcare visits every year11.
Yeast infections occur when a fungus (typically candida albicans) enters the vagina and multiplies out of control, leading to overgrowth and infection12.
Common symptoms include:
- Thick, white, clumpy vaginal discharge that looks like cottage cheese (may smell slightly yeasty or be odorless)
- Intense vaginal itching or irritation ranging from mild to severe
- Swelling, redness, or soreness around the vulva and genital area
- Burning or discomfort during urination
- Pain during sexual intercourse, especially with penetration or deep thrusting
If you're experiencing three or more yeast infections per year, these are considered recurrent yeast infections, and that's when it's especially important to identify and address contributing risk factors like IUD use13.
What's the Link Between IUDs and Yeast Infections?
Since their introduction in 1988, IUDs have only grown in popularity—and for good reason14. Beyond being over 99% effective at preventing pregnancy, they offer some serious benefits:
- Long-lasting: Protect against pregnancy for 3-10 years, depending on the type
- Hassle-free: No daily pills to remember or rings to swap out, and partners can't feel them during sex
- Cost-effective: One upfront cost covers years of contraception
- Reversible: Easily removed when you're ready to try for pregnancy
But here's the trade-off: one of the biggest drawbacks of IUD use is the increased risk of vaginal infections like yeast infections and bacterial vaginosis. Multiple studies on IUD users and candida prevalence confirm this connection. So what's going on15?
It all comes down to your vaginal microbiome.
How IUDs Disrupt Your Vaginal Flora
A healthy vaginal microbiome is dominated by protective Lactobacillus bacteria. These good bacteria produce lactic acid, which keeps your vaginal pH slightly acidic (usually between 3.8 and 4.5). While "acid" in your vagina might sound harsh, this acidic environment is actually your vagina's first line of defense. It kills harmful bacteria and keeps fungal overgrowth in check16.
But the vaginal microbiome is delicate. IUDs can disrupt this balance through several mechanisms:
1. Foreign Body Response: The presence of any foreign device in your reproductive system can trigger inflammation and cellular changes17. This inflammatory response leads to shifts in your vaginal microflora that allow candida to colonize more easily.
2. pH Balance Disruption: IUDs can alter your vaginal pH levels18. Irregular bleeding patterns (a common side-effect of both copper and hormonal IUDs, especially in the first few months) can raise vaginal pH and create an environment where yeast thrives instead of being suppressed.
3. Microbiome Changes: Research shows that IUD users often experience decreased abundance of protective Lactobacillus bacteria, especially over time19. When these beneficial bacteria diminish, candida species and other harmful microbes can overgrow without competition, leading to infection.
Prebiotic + Probiotic
Maintains vaginal pH and restores gut health.
What the Research Shows
Multiple studies have confirmed the link between IUD use and increased yeast infection risk. Here are four to know about:
- Study 1: A 2022 comparison of hormonal and non-hormonal IUDs found that 29.57% of women with copper IUDs were diagnosed with candidiasis three months after insertion, compared to 22.95% of hormonal IUD users.
- Study 2: Researchers followed 217 women without other risk factors for yeast infections. Among the 117 women who got IUDs, 20% tested positive for candida in vaginal smears—compared to only 6% of the 100 women without IUDs.
- Study 3: In a study of 150 women (108 with copper IUDs, 42 with hormonal IUDs), copper IUD users showed increased candida and mycoplasma overgrowth after one year. They also reported more vaginal discharge and pelvic pain.
- Study 4: Researchers evaluated 252 women's vaginal flora before and after hormonal IUD insertion. They found that bacterial vaginosis rates increased in the short term (3 months post-insertion), while longer durations (1-5 years) were linked with candida overgrowth. Interestingly, yeast presence in vaginal samples can actually increase during years 4 to 7 compared to the first year after insertion.
The bottom line? The link between IUDs and vaginal infections is real. The highest risk period is typically within the first three months after IUD insertion, though some women develop infections months or even years later. But that doesn't mean you need to avoid IUDs altogether, especially if you find them convenient in protecting pregnancy. It just means you need to be proactive about prevention.
Can IUDs Cause Other Types of Infections?
Yes. Because IUDs disrupt your vaginal microbiome, they can increase your risk of several types of infections beyond just yeast infections, including:
- Bacterial vaginosis (BV): One of the most common vaginal infections, BV occurs when harmful bacteria outnumber beneficial Lactobacillus20
- Sexually transmitted infections like chlamydia and gonorrhea: While IUDs don't cause STDs, the disrupted protective flora makes you more vulnerable to these infections21
- Pelvic inflammatory disease (PID): A serious infection of the reproductive organs that can lead to infertility if untreated22
What Other Risk Factors Increase Your Chances of Getting a Vaginal Yeast Infection?
We've talked about studies that link IUD use to increased risk of yeast infection and vaginal candidiasis, but it’s important to remember having an IUD doesn't guarantee you'll develop infections. Your chances go up significantly, though, if you also have any of these additional risk factors:
Reduced Vaginal Lubrication
Estrogen plays a crucial role in keeping your vaginal walls lubricated and preventing vaginal dryness. When you get a hormonal IUD, your estrogen levels can drop, and for some women, this results in vaginal dryness23.
While vaginal dryness is mostly known for making sex uncomfortable, it also makes you more susceptible to infections24. Dry, inflamed vaginal tissues make it easier for yeast and other harmful microbes to attach and multiply.
Allergic Reactions to IUD Components
In rare cases, some women experience allergic reactions to their IUD materials, whether it's the copper itself in copper IUDs or the hormone-releasing components in hormonal birth control IUDs25. This allergic reaction causes inflammation and irritation within your vagina, creating an environment where yeast can thrive.
Sexual Activity
Sex doesn't directly cause yeast infections, but certain sexual behaviors can increase your risk, especially:
- Unprotected sex with multiple or new partners
- Using unsterilized sex toys
- Finger insertion without clean hands
These activities can introduce harmful bacteria into your vagina, disrupting your microbiome and making candida overgrowth more likely. If you already have an active yeast infection, sex can also make symptoms worse due to friction and irritation26.
Allergic Reactions to IUD Components
In rare cases, some women experience allergic reactions to their IUD materials, whether it's the copper itself in copper IUDs or the hormone-releasing components in hormonal birth control IUDs. This allergic reaction causes inflammation and irritation within your vagina, creating an environment where yeast can thrive27.
Other Common Risk Factors
Additional factors that put you at higher risk for yeast infections include:
- High sugar intake: Sugar feeds yeast growth, so diets high in refined carbohydrates can worsen infections
- Medical conditions like diabetes: Elevated blood sugar creates an ideal environment for yeast
- Overuse or misuse of antibiotics: Antibiotics kill beneficial bacteria along with harmful ones
- Poor diet lacking in nutrients and whole foods
- Hormone replacement therapy: Can disrupt your natural hormone balance
- Poor genital hygiene practices like douching or using scented products
Understanding all the risk factors that apply to you is critical, especially if you are experiencing recurrent vaginal yeast infections28.
Are Vaginal Yeast Infections Treatable?
Absolutely! While yeast infections are uncomfortable and frustrating, they're easy to diagnose and highly treatable29.
Getting Diagnosed
The first step is confirming you actually have a yeast infection (and not bacterial vaginosis or another condition). Call your OB/GYN or healthcare provider to schedule an appointment. Here's what to expect:
- Your doctor will ask about your medical history, including past vaginal infections
- They'll perform a pelvic exam
- They may take a vaginal swab for lab testing to confirm the diagnosis
- If positive, you'll receive antifungal treatment
Treatment Options
The good news is that you can absolutely treat yeast infections while you have an IUD. Over-the-counter and prescription antifungal medications are safe and effective with IUDs.
There are several antifungal options available, with the most popular being:
- Topical creams and suppositories like clotrimazole (applied directly to the affected area)
- Oral tablets like fluconazole (taken by mouth)
Both work extremely well. A 2003 study published in the American Journal of Obstetrics and Gynecology found cure rates of 79.2% with oral treatment and 80.9% with topical creams. The choice really comes down to personal preference and whether you'd rather use a vaginal cream, a suppository, or take a pill.
If you're experiencing three or more infections per year despite treatment, consult your healthcare professional about additional strategies or potentially switching birth control methods.
How Can I Prevent Yeast Infections While Using an IUD?
Your vaginal health is a window into your overall wellness. And as with everything health-related, prevention beats treatment every time.
This is especially true with yeast infections. While killing off candida overgrowth is relatively straightforward, restoring a balanced vaginal microbiome takes more work. Luckily, these prevention strategies can support your vaginal flora and stop infections before they start.
Practice Good Genital Hygiene
Good vaginal hygiene includes:
- Changing out of sweaty clothes promptly after working out or swimming
- Wearing breathable cotton underwear
- Wiping front to back after using the bathroom
- Urinating after sex to flush out bacteria
- Washing your genital area with only warm water and mild, unscented soaps
- Avoiding douching, scented soaps, and harsh vaginal cleansers
Skip Tight-Fitting Clothing
Many of the hygiene practices we just mentioned are about keeping your vagina clean and dry. That's because damp, warm environments are breeding grounds for bad bacteria and yeast. Tight pants trap moisture and sweat in your genital area, increasing your chances of bacterial or fungal overgrowth. Opt for looser, breathable fabrics when possible.
Watch Your Diet
High sugar intake feeds yeast growth—literally. If you're prone to infections, focus on whole foods and reduce refined carbohydrates and added sugars. This dietary change alone can make a significant difference in preventing recurrent infections.
Take Daily Probiotics
Probiotics are beneficial bacteria. In your gut, they help with digestion. In your vagina, they're responsible for maintaining that acidic pH that keeps bad microbes at bay.
The main probiotic for vaginal health is Lactobacillus. Research shows that specific Lactobacillus strains of L. rhamnosus and L. crispatus can help restore vaginal balance and support yeast infection prevention.
Happy V's Prebiotic + Probiotic contains these clinically-studied Lactobacillus strains at their clinically effective doses. Preclinical data of our unique formula (which we list on our label so there are no secrets or surprises!) shows that Happy V is effective against the strains of Candida most associated with vaginal yeast infections, like Candida albicans.
If you have an IUD and a history of yeast infections, taking a daily probiotic like Happy V’s that’s doctor-formulated to support vaginal health ensures you're consistently supporting your body's natural defenses.
Practice Safe Sex
While yeast infections aren't classified as STIs, unprotected sex with multiple or new partners can absolutely disrupt your vaginal flora and increase infection risk. Plus, unprotected sex puts you at higher risk for actual STIs, like chlamydia and gonorrhea, which can lead to serious complications like pelvic inflammatory disease and infertility.
We're not trying to scare you away from sex, just reminding you that condoms are a simple, cost-effective way to protect your health. And even if you use condoms, peeing after sex is still a good idea. Penetration can push bacteria from your genital area into your vagina, so flushing everything out with urination helps prevent both yeast infections and UTIs.
Should I Remove My IUD If I Keep Getting Yeast Infections?
Not necessarily. Many women successfully manage yeast infections while keeping their IUD. Only consider removal if infections persist despite consistent prevention efforts and treatment, or if they significantly impact your quality of life.
Before rushing to get your IUD removed, make sure you're:
- Following all the prevention practices mentioned above
- Taking a daily probiotic with clinically-studied strains (if the label doesn’t list the exact strains of Lactobacillus or has sketchy “proprietary blends,” don’t buy it)
- Managing dietary factors like sugar intake
- Treating infections promptly and completely
If you continue to struggle with frequent infections even after implementing these strategies, talk with your healthcare professional. They can help you explore additional treatment options, identify other contributing factors, or discuss alternative methods of contraception that might work better for your body.
Final Thoughts
If you're using an IUD and struggling with recurrent yeast infections, you're not imagining the connection. The research is clear that both copper IUDs and hormonal IUDs can increase your risk of vaginal candidiasis and bacterial vaginosis. Copper IUDs appear to carry a slightly higher risk, particularly in the first year, while hormonal IUD users may see increased yeast prevalence in years 4-7 of use.
But that doesn't mean you need to rush to get your IUD removed. Start by doubling down on prevention: practice good genital hygiene, wear breathable clothing, watch your sugar intake, practice safe sex, and most importantly, add a daily probiotic to your routine.
Remember: yeast infections are treatable, and with the right prevention plan, you can keep your vaginal health on track, IUD or not.
Keep the Conversation Going
- Visit our blog for more women's health tips.
- Join our private Happy V Facebook group to hear from others who've been there.
- Explore supplements designed to support your vaginal health journey.
Disclaimer: This blog is for informational and educational purposes only and is not intended to diagnose, treat, cure, or prevent any disease. Statements about supplements have not been evaluated by the Food and Drug Administration. For more information about vaginal infections, visit the CDC or speak to a licensed healthcare provider.